What is Anal Cancer?
Let’s start with the basics. Anal cancer is a cancer that begins in the anus, the short canal at the very end of your digestive tract. The anus is only about 1.5 inches long, but it plays an important role: it’s how waste leaves your body after digestion.
The anus is made up of different types of cells. Most notably:
Squamous cells, which form a thin, skin-like lining
Gland cells, which produce mucus to keep the area lubricated
Anal cancer most often starts when squamous cells begin to grow abnormally. Over time, these abnormal cells can form a tumor and, if left untreated, spread to other parts of the body.
Anal cancer is considered rare, but rates have been steadily increasing, especially in certain communities. That’s why awareness matters.
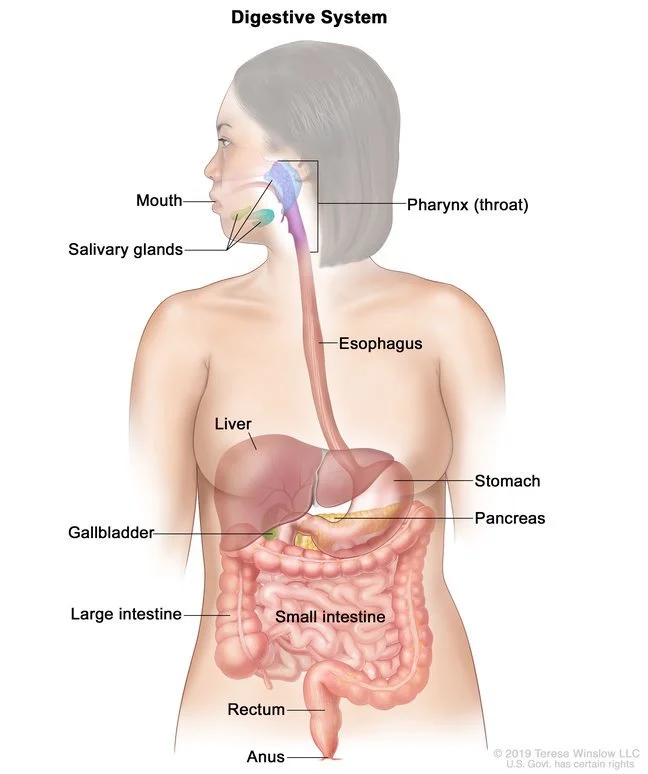
Anatomy of the Anus
Knowing how the anus works helps explain how anal cancer develops.
Here’s the quick version:
After digestion, waste moves through the large intestine into the rectum.
The anus connects the rectum to the outside of the body.
Muscles and nerves in the anus control bowel movements.
The lining of the anus is constantly renewing itself as cells grow, die, and are replaced.
When that normal cell turnover goes wrong, often due to HPV-related changes, cancer can begin to form.
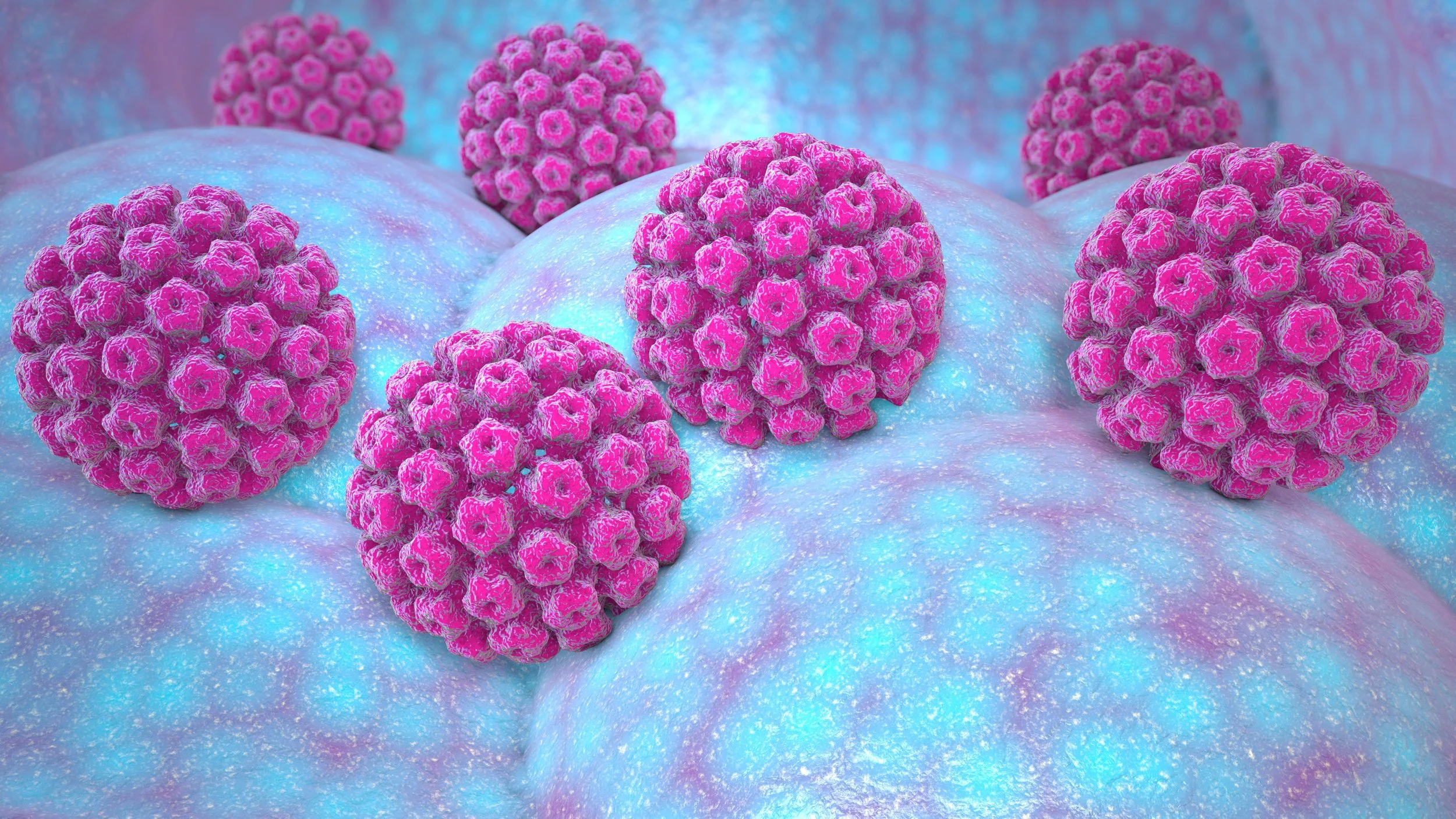
Why Anal Cancer Happens
Most cases of anal cancer are linked to human papillomavirus (HPV), a very common virus. In fact, the majority of sexually active people will have HPV at some point in their lives, often without ever knowing it. In some cases, high-risk strains of HPV can cause long-term changes in cells that may eventually lead to cancer.
People at higher risk for anal cancer include:
People with persistent HPV infections
Individuals with weakened immune systems, including people living with HIV
People who engage in receptive anal sex
LGBTQ+ individuals who face barriers to preventive care and screening
HPV vaccination is one of the most powerful tools we have to prevent anal cancer, yet access and awareness are still uneven. Closing those gaps saves lives.
How Anal Cancer Is Different From Other Cancers
Anal cancer is often grouped with gastrointestinal (GI) cancers, but it is not the same as colon or rectal cancer.
Colon and rectal cancers develop higher up in the digestive tract, where nutrients and water are absorbed.
Anal cancer affects the very end of the system and involves different cell types, risk factors, and treatments.
Because of these differences, anal cancer has its own screening approaches, prevention strategies, and treatment plans.
How Common Is Anal Cancer?
Each year, about 9,000 people in the United States are diagnosed with anal cancer. While that’s a small percentage of overall cancer cases, rates are significantly higher among certain groups, including gay and bisexual men and people living with HIV.
What matters most is this: anal cancer is often highly treatable when caught early. Awareness of symptoms, understanding your risk, and having access to affirming healthcare can make a real difference in outcomes.
Why Awareness and Prevention Matter
Anal cancer doesn’t get talked about nearly enough. Stigma, discomfort, and lack of education keep many people from asking questions or seeking care.
Here’s the truth: HPV is common, anal cancer risk is real, and prevention and early detection work!
HPV vaccination, safer sex practices, and regular conversations with a healthcare provider can dramatically reduce risk. If cost, insurance, or access is a concern, there are programs that offer low-cost or free vaccines and screenings.
Your butt deserves care, attention, and respect. Learning about anal cancer is one way to take control of your health and advocate for yourself and your community.
-
HPV and Anal Cancer – The HPV and Anal Cancer Foundation
https://www.analcancerfoundation.org
This foundation provides information on anal cancer prevention, treatment, and support for individuals affected by anal cancer.Cancer Support Community: Understanding Anal Cancer
https://www.cancersupportcommunity.org
Offers support services, educational resources, and counseling for individuals and families affected by anal cancer.LGBTQ+ Cancer Resources – National LGBT Cancer Network
https://www.cancer-network.org
Focuses on cancer resources and support specifically for LGBTQ+ individuals, including those at higher risk of anal cancer.CDC HPV Vaccine Information
https://www.cdc.gov/hpv/parents/vaccine.html
Provides information on HPV vaccination as a preventive measure, including guidance on vaccine access and recommendations.American Sexual Health Association (ASHA): HPV and Men
https://www.ashasexualhealth.org/hpv-and-men
Focuses on HPV-related health issues in men, including those at increased risk for anal cancer. -
American Cancer Society: What Is Anal Cancer?
https://www.cancer.org/cancer/anal-cancer/about/what-is-anal-cancer.htmlNational Cancer Institute: Anal Cancer Treatment (PDQ®)–Patient Version
https://www.cancer.gov/types/anal/patient/anal-treatment-pdqCenters for Disease Control and Prevention (CDC): HPV and Cancer
https://www.cdc.gov/cancer/hpv/statistics/cases.htmAmerican Society of Clinical Oncology (ASCO): Anal Cancer - Overview
https://www.cancer.net/cancer-types/anal-cancer/introductionNational Comprehensive Cancer Network (NCCN) Guidelines for Patients®: Anal Cancer
https://www.nccn.org/patients/guidelines/anal/index.html
